LGD 2004 (1) - David P Fidler
Germs, Norms and Power: Global Health's Political Revolution
David P Fidler
Professor of Law and
Ira C Batman Faculty Fellow,
School of Law, University of Indiana,
and
Senior Faculty Fellow,
Center for the Law and the Public's Health,
Georgetown and John Hopkins Universities, USA
dfilder@indiana.edu
Global health has undergone a political revolution in the last fifteen years. From a neglected area of international politics, public health has emerged prominently on the agendas of many policy areas in international relations, including national security, international trade, economic development, globalization, human rights, and global governance. This political revolution has occurred because of crises posed by infectious diseases (germs), ferment in thinking about policy responses to these crises (norms), and the need to engage material resources and capabilities to contain and mitigate the pathogenic threat (power). This article examines each aspect of global health’s political revolution to understand how germs, norms, and power converge in a manner that illuminates not only the global struggle to protect health but also 21st century international politics. The analysis of the growing infectious disease threat examines both the threat of biological weapons and emerging and re-emerging infectious diseases. The exploration of the ferment in norms probes three different conceptual frameworks that have emerged to structure responses to pathogenic threats. The consideration of the role of power focuses on the impact on global health’s political revolution of the preponderance of US power in today’s international system. The article also examines dilemmas that appear in the germs, norms, and power elements of the political revolution that call into question the meaning and sustainability of global health’s new-found importance in foreign policy and international relations. Global health’s political revolution remains enigmatic and incomplete, meaning that both danger and opportunity await this area of world politics.
Keywords: Bioterrorism, Foreign Policy, Global Health Global Health Governance, Global Public Goods for Health, Globalization, Governance, Infectious Diseases, National Security, Norms, Power, Public Health, Right to Health, Weapons of Mass Destruction, Westphalian, Post-Westphalian, World Health Organisation
This is a refereed article published on 4 June 2004.
Citation: Fidler, D, 'Germs, Norms and Power: Global Health's Political Revolution', Law, Social Justice & Global Development Journal (LGD) 2004 (1), <http://elj.warwick.ac.uk/global/04-1/fidler.html>. New citation as at 15/07/04: <http://www2.warwick.ac.uk/fac/soc/law/elj/lgd/2004_1/fidler/>.
Dramatic change marks the history of health as an issue in international relations. Health’s emergence as a foreign policy concern in the mid-19th century, when European nations began to confront cooperatively the cholera menace, represents one such dramatic transition in how health was conceptualised and approached internationally. Subsequent treaties and international health organisations also transformed health as a foreign policy concern. Technological developments, especially antibiotics and vaccines, also produced change for public health globally.
These examples of changes in international health reveal and obscure. They reveal that health has long been a foreign policy issue. Given this history, ‘health as foreign policy’ is not a novel idea. The examples obscure that health has historically been relegated to the foreign policy fringe of technical assistance and humanitarianism. The lack of interest in health by those studying foreign policy and international relations compounded the neglect (Lee, K and Zwi, A, 2003, p 13; Kickbusch, I, 2003, p 192). Given this situation, ‘health as foreign policy’ was not an important diplomatic activity.
Dramatic change has, however, again visited health as an issue in international relations. In the past decade, health emerged from obscurity and neglect to affect many foreign and international policy agendas. Health now features prominently in debates concerning national and homeland security, international trade, economic development, globalisation, human rights, and global governance. The attention health has received in the past ten years in national and international politics is unprecedented. Kickbusch (2003, pp 192-93) captured this change:
The protection of health is no longer seen as primarily a humanitarian and technical issue relegated to a specialised UN agency, but more fully considered in relation to the economic, political, and security consequences for the complex post-Cold War system of interdependence. This has led to new policy and funding initiatives at many levels of governance and a new political space within which global health action is conducted.
Health as a global issue has undergone a political revolution in the last decade. Health’s emergence into the ‘high politics’ of international relations is a complicated and controversial development. Global health’s political revolution means that traditional approaches to, and attitudes about, public health have been ripped from their moorings and set afloat on a volatile sea. This article examines global health’s political revolution by analyzing its components and how they relate to each other in an attempt to understand the meaning of this revolution for global health’s future.
Revolutions constitute radical changes within existing political systems, and they typically involve three elements: (1) a crisis with the status quo; (2) a challenge from normative ideas different from those operative in the existing system; and (3) the application of material power to install the new ideas as the basis for future action. The article explores each of these elements in connection with global health’s transformation as an issue in international relations.
The crisis comes from threats posed by infectious diseases (germs). The mounting microbial menace has stimulated ferment among policy responses that seek to supercede existing strategies and alter how state and non-state actors address pathogenic threats (norms). The competing ideas require material resources and capabilities to contain and mitigate the microbial challenge to health (power).
How germs, norms, and power converge shapes the nature of global health’s political revolution. I argue that the political revolution remains enigmatic, and the enigma raises questions about the revolution’s impact and sustainability. Global health’s political revolution serves as a window on the future of not only the protection of health but also 21st century world politics.
The growing threat from the microbial world has triggered global health’s political revolution. Although concerns about the globalization of non-communicable diseases have increased (Beaglehole, R and Yach, D, 2003), the threat posed by pathogenic microbes has driven the rise of global health as a foreign policy issue. The crisis in the status quo in the last decade includes both naturally occurring infectious diseases and the use of microbes as weapons. The germ threat can be captured by looking at two axes, the ‘axis of evil’ and the ‘axis of illness,’ that communicate the dangers germs pose today.
2.1 Biological Weapons and Bioterrorism
The impact on public health of fears about the proliferation and use of biological weapons has been significant in the 1990s and early 2000s. These fears were growing before the anthrax attacks in the United States in 2001, and these attacks accelerated fusion between public health and national security in policy efforts against weapons of mass destruction (WMD). Prior to the last decade, public health was not part of national security and foreign policy on WMD because the approach to the WMD threat was arms control (Fidler, D, 2003a). The WMD threat, especially bioterrorism, has changed policy such that public health is now a central component of foreign policy, national security, and homeland security efforts against the proliferation and use of WMD generally and bioweapons specifically.
In the United States, the WMD and bioterrorism threats have affected policy from strategic doctrine to local public health preparedness. The United States has located the bioterrorist threat within a strategic framework of U.S. national security that President Bush controversially termed the ‘axis of evil’ (Bush, G, 2002). Putting aside the rhetoric, the substantive components of the axis form a post-9/11 strategic doctrine that identifies threats to US national and homeland security and provides a blueprint for the exercise of US power. The axis of evil highlights the policy interdependency of three factors: repressive regimes, international terrorism, and WMD (Bush, G, 2002) (Figure1).
This strategic doctrine communicates that WMD proliferation and their use by state and non-state actors constitutes a direct security threat to the United States. The doctrine resonates with concerns about WMD generally and bioterrorism specifically that developed before George W. Bush was elected president. The anthrax attacks of 2001 demonstrated bioterrorism’s potential to inflict damage on a country.
Figure 1: The Substantive Elements of the 'Axis of Evil'
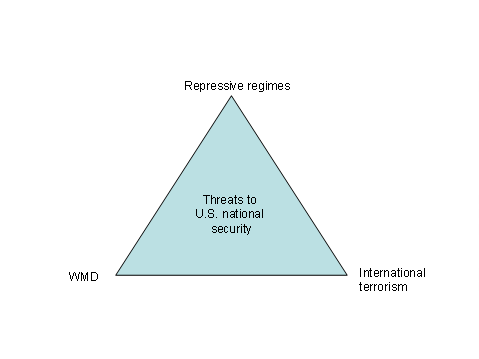
Source: Fidler, D, 2003
As a strategic doctrine, the ‘axis of evil’ has generated diverse responses at different policy levels. The Bush administration’s strategy of pre-emptive self-defence against states that possess or pursue WMD and that support international terrorism is one policy response (White House, 2002a, p 15). In terms of public health, the doctrine supports the significant effort underway in the United States for public health preparedness against future attacks using bioweapons (Office of Homeland Security, 2002, pp 43-44). Recognition of the bioweapons threat extends beyond the United States because the World Health Organisation (WHO) has also become engaged with public health preparedness against the intentional use of microbes as part of strengthening ‘global health security’ (WHO, 2002a, p 12).
2.2 Emerging and Re-Emerging Infectious Diseases
The proliferation and use of bioweapons is only one aspect of the growing threat microbes present. Microbial dangers also include challenges created by naturally occurring infectious diseases (Institute of Medicine, 2003). Concern about emerging and re-emerging infectious diseases populated public health literature in the 1990s (eg Institute of Medicine, 1992; US CDC, 1994; Garrett, 1995, National Science and Technology Council, 1995; US CDC, 1998; WHO, 1999; Farmer, 1999). Contributing to the worries about naturally occurring infectious diseases was the HIV/AIDS pandemic, which reached shocking proportions in parts of the developing world by the end of the 20th century (UNAIDS, 2001). Other fears also existed, including the development of antimicrobial resistance in pathogens in many parts of the world (WHO, 1999).
In other works, I developed the ‘axis of illness’ to identify key factors that converge to produce the dangers naturally occurring infectious diseases pose (eg Fidler, D, 2003b; Fidler, D, 2003c). Analyses of emerging and re-emerging infectious diseases often produce lists of factors that contribute to microbial emergence and spread. In 1992, the Institute of Medicine’s seminal report on emerging microbial threats to health in the United States contained six such factors (p 47): human demographics and behaviour; technology and industry; economic development and land use; international travel and commerce; microbial adaptation and change; and breakdown of public health measures. The Institute of Medicine’s 2003 report (pp 4-7) communicated a sense of the worsening of the threat because it listed thirteen factors behind infectious disease emergence and re-emergence (Table 1).
Table 1. Institute of Medicine’s 2003 List of Factors Behind Infectious Disease Emergence and Re-Emergence
|
|
The ‘axis of illness’ represents one way to conceptualise the threat posed infectious disease emergence and re-emergence. The axis of illness contains five categories that interact to stimulate the emergence and spread of infectious diseases: microbial resilience; human mobility; social determinants of health; globalization; and collective action problems (Figure 2). More specific factors identified by, for example, the Institute of Medicine slot into one or more of these five categories (Table 2).
‘Microbial resilience’ captures the importance of microbial, genetic, and biological factors that drive pathogenic evolution and its relationship to humans. ‘Human mobility’ emphasises the roles international trade, travel, and migration play in disease emergence, including the contributions technology and industry make in increasing the speed, scope, and impact of human mobility. ‘Social determinants of health’ focuses on underlying problems that foster microbial penetration of populations. Social determinants of health face pressure from the other elements of the axis of illness and are adversely affected by factors, such as the breakdown of public health capabilities, which undercut the ability to protect and promote health.
‘Globalization’ refers to factors that accelerate economic, technological, industrial, and cultural interconnectedness in ways that de-territorialise human behaviour and the milieu in which humans and microbes interact. ‘Collective action problems’ refer to the governance challenges created by infectious disease emergence at local, national, and global levels. When the Institute of Medicine (2003, pp 107-121) identifies the breakdown in public health measures as a risk factor, it focuses attention on government and governance failures on public health. Responding to resurgent infectious disease requires successful collective action both within and among states.
2.3 The Microbial Challenge and World Politics
More could be said about the axes of evil and illness because they attempt to simplify complex challenges, but my objective is to communicate generally the growing threats to global health created by pathogenic microbes. The threats framed by the axes have triggered the political revolution in global health because these threats challenged and overwhelmed status quo approaches to bioweapons and global infectious disease control. The germ threats have stripped global health’s ancien régime of credibility, forcing states, intergovernmental organisations, and non-state actors to re-conceptualise public health governance nationally and globally.
The perturbation in world politics caused by the microbial challenge can be glimpsed in how infectious diseases have become an issue on virtually every major political agenda today (Table 3). This type of political impact is unprecedented for public health’s place in world affairs.
Figure 2: The Axis of Illness
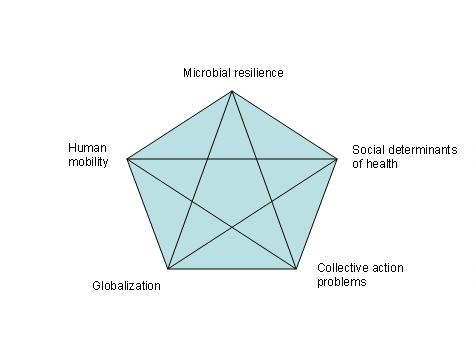
Source: Fidler, 2004
Table 2. Factors of Emergence in the Five Categories
|
Category |
Factors from Institute of Medicine (2003) |
|
Microbial resilience |
Microbial adaptation and change; human susceptibility to infection |
|
Human Mobility |
International trade and travel; human demographics and behaviour; technology and industry |
|
Social determinants of health |
Poverty and social inequalities; war and famine; climate and weather; human demographics and behaviour; technology and industry |
|
Globalization |
Economic development and land use; technology and industry; changing ecosystems; human demographics and behaviour |
|
Collective action Problems |
Lack of political will; intent to harm; breakdown of public health measures; poverty and social inequalities; war and famine |
Source: Fidler, D, 2004
Table 3. Infectious Diseases and World Politics
|
Area of World Politics |
Infectious Disease Examples |
|
National security |
Threat of proliferation and use of biological weapons |
|
Foreign policy |
Threat of bioterrorism and controversies over funding HIV/AIDS efforts in the developing world |
|
International trade |
Access to antiretrovirals and other essential medicines for infectious disease treatment and the TRIPS Agreement |
|
Economic development |
Commission of Macroeconomics and Health’s arguments that infectious disease control should be at the centre of strategies for economic development |
|
International aid |
The importance of reducing infectious disease morbidity and mortality in connection with the Millennium Development Goals |
|
Human rights |
Appointment of a Special Rapporteur on the Right to Health, who is interested in the right to health issues involving infectious diseases |
|
International law |
WHO’s efforts to revise the International Health Regulations, the only rules on infectious diseases binding on WHO member states |
|
Globalization |
SARS outbreak reinforcing the powerful force globalization represents in spreading infectious diseases |
|
Global governance |
Creation of public-private partnerships to address global infectious disease problems |
|
Global civil society |
Global NGOS, such as Médecins Sans Frontières, have increased their activism with respect to infectious disease problems |
|
Ideology |
Infectious disease problems have stimulated ideological controversies with respect to neo-liberalism and China’s handling of its HIV/AIDS and SARS outbreaks |
The germ threat has forced public health and other policy communities to respond to the microbial menace. The responses that have developed reveal ferment in thinking about global health, particularly with respect to what norms should guide reaction to the threats from bioweapons and emerging infectious diseases. This ferment suggests recognition of the need to ‘man the barricades’ against the germ threat, but it does not indicate consensus on how to man the barricades. This section explores three normative perspectives about global health that embody competing conceptualisations of the germ threat and how to address it.
Before analysing the norms competing for attention today, some historical background is necessary on how global health endeavours were conceptualised in past eras. In other publications, I identified two over-arching perspectives on infectious disease control specifically and public health generally: the Westphalian[1] and post-Westphalian perspectives (Fidler, D, 2003b; Fidler, D, 2003c; Fidler, D, 2004). The Westphalian perspective dominated global health from the origins of international health diplomacy in 1851 until the end of World War II. The post-Westphalian perspective was prominent in the post-World War II period and enjoyed its halcyon moment at the end of the 1970s.
The Westphalian approach to infectious diseases centred on the sovereign state and conceptualised pathogens as exogenous threats to the state’s national interests and power. The Westphalian perspective developed with respect to naturally occurring infectious diseases only because bioweapons were not a public health concern during the first 100 years of international health diplomacy.
Infectious diseases provided two types of exogenous threats to states. First, a state faced increased disease importation as the scope and speed of international trade and travel grew. As European countries learned in their battles with cholera in the 19th century, both national improvements (eg sanitation reform in urban areas) and international cooperation (eg international surveillance) were required to reduce a country’s vulnerability to disease importation.
Second, infectious diseases posed exogenous threats to a state’s national interests and power through the burdens imposed on its trade and commerce by other countries’ trade-restricting health measures, namely quarantine. As international health historians have observed, the burdens on international trade created by an uncoordinated system of national quarantine measures provided the greatest impetus for international cooperation on infectious diseases (Goodman, N 1971, p 389; Howard-Jones, N, 1975, p 11).
The Westphalian perspective on infectious diseases seemed to contain contradictory objectives: (1) reduce exogenous disease threats through improved national defences against disease importation; and (2) reduce the friction that national defences against exogenous disease threats create for trade and commerce. International cooperation was the only way to reconcile these objectives, as the development of international health diplomacy in the latter half of the nineteenth and first half of the 20th century illustrates.
The pattern international health cooperation followed for approximately a century adhered to the core principles of Westphalian international politics: state sovereignty; non-intervention in the domestic affairs of other states; and regulation of sovereign interactions through consent-based rules of international law. Through treaties and international health organisations, states built a horizontal regime that sought to regulate cross-border microbial traffic and to minimise the impact of health measures on international trade (Figure 3). This regime showed no interest in infectious disease problems inside states because that issue was off-limits under the principles of sovereignty and non-intervention.
The post-Westphalian approach to public health and infectious diseases developed after World War II, and this approach received its first comprehensive presentation in the WHO Constitution, which entered into force in 1948 (WHO,1948). The post-Westphalian approach rejected framing public health in terms of exogenous disease threats to a state’s national interests and power. Rather, the post-Westphalian approach focused on the individual’s fundamental right to the highest attainable standard of physical and mental health (WHO,1948, p 1). The post-Westphalian perspective argued that the fulfilment of this right required seeing the health of individuals, peoples, and countries as interdependent (WHO, 1948, p 1). Such health solidarism created the need and opportunity for redistributive justice to raise the health conditions of the poorest and most vulnerable populations (WHO,1948, p1).
Te post-Westphalian conceptualisation radically re-oriented international health, shifting the focus away from horizontal, state-centric strategies toward vertical, rights-based approaches designed to reduce disease morbidity and mortality at their sources within countries (Arhin-Tenkorang, D and Conceiçao, P, 2003, pp 485-87) (Figure 4). The post-Westphalian strategy reached its zenith at the end of the 1970s with the twin triumphs of the global eradication of smallpox (Koplow, D, 2003, pp 21-31) and the adoption of the Health for All strategy of primary health care (WHO, 1978). The emergence of the HIV/AIDS pandemic in the 1980s strengthened the momentum of post-Westphalian strategies as the global effort against the pandemic adopted a human rights approach (Gruskin, S and Tarantola, D, 2003).
Figure 3: Westphalian Governance of Infectious Diseases
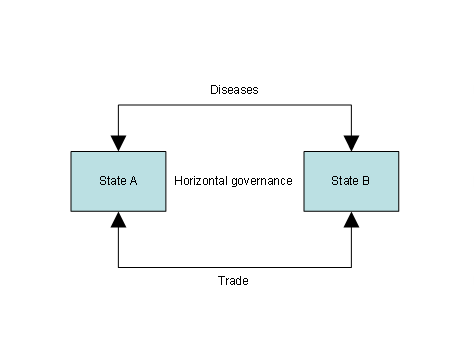
Source: Fidler, D, 2003b
Figure 4: Vertical Governance
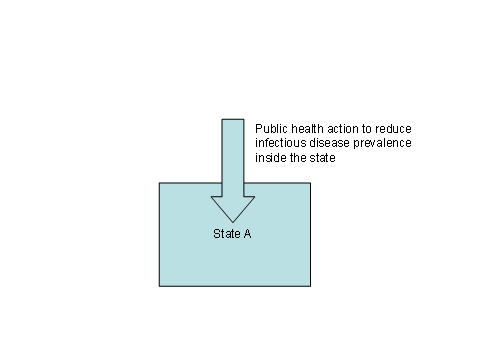
Source: Fidler, D, 2003b
These descriptions of the Westphalian and post-Westphalian frameworks are important because today’s normative ferment in the face of the mounting microbial threat resonates with both these perspectives. Global health’s political revolution contains, thus, strong traces from its pre-revolutionary period. Two of the three major normative frameworks prominent in global health discourse descend from the Westphalian and post-Westphalian perspectives. The third framework navigates between the contemporary versions of the Westphalian and post-Westphalian strategies.
After fading during the post-World War II period, the Westphalian perspective has returned as one of the most prominent features of global health’s political revolution. As described earlier, the Westphalian perspective conceptualised infectious diseases as exogenous threats to a state’s national interests and power in two respects: (1) a direct threat through disease importation; and (2) an indirect threat to trade and commercial interests arising from other nations’ trade-restricting health measures. Neo-Westphalianism contains the same conceptualisation, but it includes new features not present in earlier times.
Concerns about emerging infectious diseases have focused on the increased likelihood of infectious disease importation and the threat such importation poses to the nation’s public health and economic opportunities (eg Foege, W, 2003). Part of the increasing policy attention the United States and other countries pay to global health today flows from conceptualising infectious diseases as exogenous threats to national health and economics (eg, Kassalow, J, 2001).
The old Westphalian concern that foreign nations’ trade-restricting health measures will harm a country’s national interests and power also has resurfaced in the last decade. This concern developed with respect to national quarantine measures, but the contemporary battleground has been in connection with international trade and the protection of intellectual property rights of pharmaceutical companies. The HIV/AIDS crisis in developing countries, particularly sub-Saharan Africa, has embroiled developed countries with major research-based pharmaceutical industries in battles with developing-country governments and non-governmental organisations about patent protection for anti-retrovirals standing in the way of increasing access to these drugs (Thomas, C, 2003).
Just as in the old days, the national actions of foreign governments taken to address health problems are perceived by other states as harming their interests in promoting trade and commercial interests. Infectious diseases generate friction and controversy in the international economic system. Neo-Westphalianism conceptualises infectious diseases in foreign countries as potential indirect threats to the promotion of a state’s national interests and power in international trade and commerce.
Neo-Westphalianism includes two features not present in its older manifestation, both of which raise public health into the national security realm. The original Westphalian perspective never conceptualised exogenous disease threats as national security threats. In other words, infectious diseases were a foreign policy but not a national security issue. Global health’s political revolution produces this new conceptualisation: infectious diseases are perceived to represent direct and indirect threats to a state’s national security.
The direct threat infectious diseases pose to national security comes from bioweapons. As illustrated by the axis of evil, the United States believes that the proliferation and use of bioweapons and other WMD by states or terrorists constitute national security dangers (White House, 2002a). The bioweapons threat has brought the Westphalian conceptualisation of infectious diseases back to the forefront of global health because this threat fits seamlessly into the structure and dynamics of Westphalian international relations (Fidler, D, 2003b). Public health preparedness for potential bioweapons use has, thus, become a central concern of national and homeland security policy in the United States (White House, 2002b; Office of Homeland Security, 2002). National public health capabilities have ‘rarely, if ever, been defined as a national security issue’ (Contagion and Conflict, 2000, p vii).
The indirect national security threat infectious diseases pose arose in connection with the devastation HIV/AIDS was wreaking in many developing countries. In a move also unprecedented in US national security policy, the Clinton administration argued that severe infectious disease problems in foreign countries, such as those in sub-Saharan Africa, could constitute a threat to US national security because the outbreaks could destabilise countries and regions to the detriment of US strategic, political, and economic objectives (National Intelligence Council, 2000). The scale of the HIV/AIDS pandemic gave this novel national security argument plausibility, even if not everyone was convinced of the argument (eg Zelikow, P, 2000, p 154). This conceptualisation of infectious diseases as an exogenous threat was not part of the older Westphalian framework, but it nevertheless flows from the Westphalian principle of viewing infectious diseases as exogenous threats to a nation’s interests and power.
Under neo-Westphalianism, manning the barricades of global health is necessary because the germs constitute exogenous threats to a state’s national interests, power, and security. The objective of manning the barricades is to ensure that infectious diseases do not undermine the country’s power, security, and pursuit of economic objectives overseas. Cooperation with other countries and intergovernmental organisations may be required, but cooperation bears no political significance beyond supporting a country’s attempts to strengthen its national security, economy, and foreign policy objectives against microbial challenges.
3.3 Contemporary Post-Westphalianism
Global health’s political revolution has also seen contemporary manifestations of the post-Westphalian conceptualisation of infectious diseases as threats to human rights, health solidarism between countries, and universal justice. These manifestations have been most obvious in the national and international battles fought over access to essential medicines to treat infectious diseases. These battles rejuvenated interest in, and advocacy for, the right to health first proclaimed in the WHO Constitution and at the heart of the Health for All strategy launched in the late 1970s. Evidence for this new global focus on the right to health can be seen in the UN’s issuance of a general comment on the right to health in 2000 (Committee on Economic, Social, and Cultural Rights, 2000) and appointment of a Special Rapporteur on the Right to Health in 2002 (Hunt, 2003).
The post-Westphalian tenets of health solidarism and redistributive justice also form part of the normative ferment of global health’s political revolution. The global interconnectedness highlighted by the axis of illness supports contemporary post-Westphalian arguments that, when it comes to infectious diseases, the world is a global village. In the global village, principles in the WHO Constitution (WHO, 1948, p 1) ring prophetically in the early 21st century: (1) ‘[t]he health of all peoples is fundamental to the attainment of peace and security and is dependent upon the fullest cooperation of individuals and States’; (2) ‘[u]nequal development in different countries in the promotion of health and control of disease, especially communicable disease, is a common danger’; and (3) ‘[t]he extension to all peoples of the benefits of medical, psychological and related knowledge is essential to the fullest attainment of health.’
While the threat of bioweapons heavily influences neo-Westphalianism, contemporary post-Westphalianism focuses on naturally occurring infectious diseases. The UN Special Envoy for AIDS in Africa called the normative divergence between policy concern for WMD and for HIV/AIDS ‘the grotesque obscenity of the modern world’ when he assailed the money being poured into fighting the axis of evil compared to the neglect of a pandemic that kills millions every year (Kessler, G and Stein, R, 2003, p A24). Contemporary post-Westphalianism also urges the manning of the global health barricades, but this call to arms shares no normative common ground with the neo-Westphalian conceptualisation of the global health endeavour.
3.4 A Third Way? Global Health Governance and Global Public Goods for Health
A third normative framework has appeared as part of the ferment in thinking about global health’s political revolution that focuses on the concepts of ‘global health governance’ (GHG) (eg Dodgson, R, Lee, K, and Drager, N, 2002) and ‘global public goods for health’ (GPGH) (eg Smith, R et al, 2003). The GHG idea promotes the vision of a different political process for global health, while the GPGH concept advances the vision of a new substantive objective for global health. In many respects, this strategy navigates between neo-Westphalianism and contemporary post-Westphalianism. The strategy is procedurally post-Westphalian because it rejects a state-centric focus but substantively is not wed to the right-to-health conceptualisation of global health.
The Westphalian framework produces ‘international governance,’ or governance undertaken strictly by state actors. ‘Global governance’ promotes the incorporation in governance processes of non-state actors, including non-governmental organisations (NGOs) and multinational corporations (MNCs). GHG stands for the proposition that health governance must include not only state actors but also non-state actors. The break with the Westphalian model comes in the assertion that non-state actors are necessary and legitimate governance participants.
The GHG idea does not, however, depend on acceptance of the right to health specifically or any human rights framework generally. Pursuing GHG may make sense in connection with increasing public health’s contribution to national security and prospects for achievement of the right to health. GHG mechanisms have the potential, therefore, of drawing support from both neo-Westphalianism and contemporary post-Westphalianism.
The GPGH concept developed out of interest in ‘global public goods,’ or goods that exhibit non-excludability and non-rivalry in consumption on a global basis (Kaul, I, Grunberg, I, and Stern, M, 1999). GPGH are, conceptually, post-Westphalian in pushing states to think beyond narrow, state-centric interests. GPGH do not, however, theoretically rely on the right to health, the centre of gravity for post-Westphalianism.
The ‘public goods’ framework arises from economics rather than rights-based discourse. In economic theory, a public good is an economic good that will not be produced without government intervention because the incentives or resources for private actors are insufficient. Put another way, public goods arise from market failures. Advocacy for policy interventions to produce public goods neither require nor reject a rights-based foundation. GPGH can be supported, thus, on both utilitarian and deontological grounds, providing opportunity for radically different conceptual perspectives to converge on a common policy.
The response to the global outbreak of severe acute respiratory syndrome (SARS) illustrates conceptual and concrete aspects of the GHG and GPGH ideas (Fidler, D, 2004). Prior to the SARS outbreak, one of WHO’s key proposals for revising the international regime on infectious disease control was the formal incorporation of non-governmental information in global surveillance (WHO, 2002b). This proposal sought to move surveillance from international to global governance by expanding the sources of information to include state and non-state actors. The power of this move toward GHG was demonstrated in the SARS outbreak because access to non-governmental information proved vital in WHO’s global response, especially with respect to China, the epicentre of the epidemic (Fidler, D, 2004).
The SARS crisis revealed the emergence of GHG in another, perhaps even more radical, context. Under Westphalian international governance, international organisations did not exercise independent power because member states constrained what the organisations could and could not do. During the SARS outbreak, WHO exercised independent power by issuing a global alert, emergency travel advisory, and geographically specific travel recommendations without express authorisation from the WHO Constitution, the International Health Regulations, or the member states directly affected. WHO member states acquiesced to these WHO actions at the time they were taken and then formally directed the WHO Director-General at the 2003 World Health Assembly to issue similar alerts in the future when necessary (WHO, 2003). Complaints made about WHO’s actions, such as those by Canada concerning the travel recommendations against Toronto, did not question WHO’s authority to act in these ways but merely challenged the application of such authority in a particular context.
The SARS outbreak revealed the development of a radically new governance context for global infectious diseases (Fidler, D, 2004). WHO’s power to collect information from non-governmental sources and its independent power to issue global alerts, advisories, and recommendations created a GHG pincer operating against sovereign states (Figure 5). This governance pincer transforms how states will exercise their sovereignty during infectious disease outbreaks and constitutes evidence of global health’s transition to a new governance environment.
Figure 5: The Global Health Governance Pincer
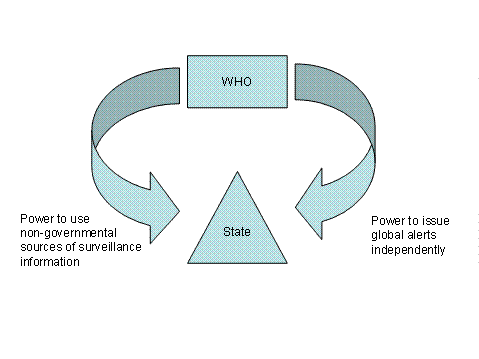
Source: Fidler, D, 2004
The SARS epidemic also illustrated the power of the GPGH concept. During the crisis, WHO led global efforts to produce information and knowledge related to the outbreak and to make such information and knowledge globally accessible. In short, WHO crafted the production of GPGH. GPGH were produced in three major areas: (1) surveillance data on SARS cases; (2) information on the best clinical practices for treating and managing SARS patients; and (3) basic scientific research about the causative agent of SARS. In each area, what happened during SARS was unprecedented. States, intergovernmental organisations, and non-state actors collaborated in the crisis production of globally accessible ‘public goods’ that contributed to the successful containment of this outbreak. The containment of SARS could itself be viewed as a GPGH given the global danger SARS presented.
The GHG and GPGH aspects of the SARS outbreak do not conceptually fall within neo-Westphalianism or contemporary post-Westphalianism. The state-centrism of neo-Westphalianism does not, for example, mix with the GHG developments that occurred during the SARS epidemic because of the way such developments transform the context in which states exercise sovereignty. Similarly, GHG and GPGH developments during the SARS crisis do not depend on post-Westphalianism’s right-to-health focus. Countries fearful of SARS’ impact on their populations and economies supported production of SARS-related GPGH because such goods helped protect national interests and power.
GHG and GPGH offer the promise of common objectives pursued through divergent conceptualisations of the infectious disease threat. GHG and GPGH do not produce normative convergence but allow for practical concurrency with respect to addressing global infectious disease threats. The GHG and GPGH concepts create the possibility for ‘unity in diversity’ concerning responses to the germ threat. The traction such concurrency provides can be seen in the support GHG and GPGH have received from states, international organisations, and non-state actors. The proliferation of public-private partnerships in the infectious disease area, which WHO (2002a, p 22) claims has reshaped the landscape of global infectious disease policy, connects to both the GHG and GPGH concepts. For example, the Global Fund to Fight AIDS, Tuberculosis, and Malaria (Global Fund) constitutes a high-profile GHG effort the objective of which is to produce the GPGH of reducing global morbidity and mortality of three killer infectious diseases (WHO, 2002a, p 23).
Despite examples of GHG and GPGH having policy impact, questions remain about the extent of productive concurrency these ideas can achieve. The concurrency can be expansive or narrow, depending on how neo-Westphalianism, contemporary post-Westphalianism, and the GHG/GPGH strategy achieve synergy (Figure 6). The key variable in determining the extent of the concurrency will be the third component of a revolution: how material power is exercised in relation to competing normative ideas.
4. From Germs and Norms to Power
The growing germ threat and the normative ferment about responding to the threat bring the final factor in global health’s political revolution into play: power. Revolutions are struggles for power between the forces of the status quo and the forces of radical change. The overthrow of the old by the new requires the exercise of superior power. Effective responses to the global threat of pathogenic microbes also require the harnessing of material capabilities, or put another way, the application of power for global health purposes.
Recognition of the microbial menace and the related normative ferment in thinking about global health has occurred during a time in which the United States emerged as the world’s hegemon, creating what some perceive is a ‘unipolar’ world. As the Bush administration argued, ‘The United States possesses unprecedented—and unequaled—strength and influence in the world’ (White House, 2002a, p 1). Both the axis of evil and the axis of illness exist in a world in which US power is preponderant.
Figure 6: Concurrency in Global Infectious Disease Policy
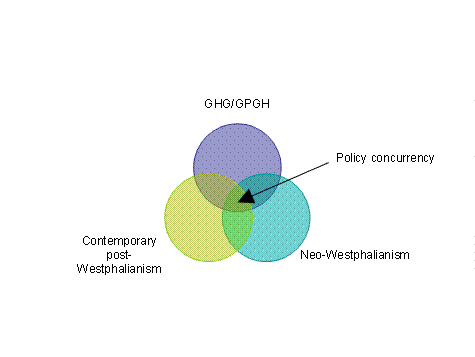
The simultaneous growth of the germ threat and the rise of the United States to hegemonic status have placed U.S. power at the centre of concern in global health’s political revolution. The last decade has witnessed many attempts to persuade the hegemon to embrace global health more robustly than it has done in the past (eg, Institute of Medicine, 1997; National Intelligence Council, 2000; Kassalow, J, 2001; Ban, J, 2001; Brower, J and Chalk, P, 2003; Campbell, K and Zelikow, P, 2003). Much of this literature resonated with neo-Westphalianism as arguments sought to convince the US government that global health and infectious disease control are in the ‘enlightened self-interest’ of the United States. The sub-title of the Institute of Medicine’s 1997 report on America’s Vital Interest in Global Health captured the nature of these appeals to the self-interest of the United States: ‘Protecting Our People, Enhancing Our Economy, and Advancing Our International Interests.’
The importance of US power can also be seen in literature critical of the U.S. approach toward global health issues generally and infectious disease problems specifically. The time, energy, and ink devoted to critical analysis of US policy on global infectious disease problems, especially HIV/AIDS, underscores the US hegemonic position. The combination of the severity of the pathogenic threat and the preponderance of US power makes the United States something of an ‘indispensable nation’ concerning the direction of global health’s political revolution.
Health as an issue in US foreign policy has, historically speaking, been considered a humanitarian and technical endeavour not of central importance to US security, interests, and power. The first comprehensive attempt to elevate health as a matter of U.S. foreign policy occurred during the Carter administration. At the beginning of his term, President Carter ordered a review of U.S. policy on international health (White House, 1978, p xxiv). This review sought to give health a more prominent role in U.S. foreign policy. The Carter administration justified this elevated role for health through appeals to U.S. economic, security, and political interests and to human rights, particularly the human right to health. Health as foreign policy to President Carter meant appealing to both Westphalian and post-Westphalian conceptualisations of health problems, but Carter’s emphasis was on the human right to health: ‘The right to health and our Nation’s moral commitment to help guarantee that right form an integral part of the foreign policy of the Carter Administration’ (White House, 1978, p 1).
President Carter’s elevation of health did not resonate with the foreign policies of the next two administrations, and health did not become an important U.S. foreign policy concern again until the Clinton administration. Rather than following Carter’s emphasis on the right to health, the Clinton administration conceptualised infectious diseases as exogenous threats to U.S. national interests, power, and security (National Science and Technology Council, 1995; National Intelligence Council, 2000). Neo-Westphalianism came of age during Clinton’s terms because his administration framed the threats from emerging infectious diseases and bioweapons according to the Westphalian approach. Although the Clinton administration was not hostile toward the right to health, this core of post-Westphalianism did not feature in the administration’s attempts to increase the profile of health as a U.S. national security and foreign policy concern.
Unlike the Republication administrations that followed Carter, the Bush administration has elevated health as a national security and foreign policy concern beyond what the Carter and Clinton administrations attempted. The fact that a neo-conservative, unilateralist-minded administration has integrated health concerns into its national security and foreign policies in a high-profile manner is evidence of the magnitude of the germ threat and the reality of global health’s political revolution.
The Bush administration has adopted neo-Westphalianism in its approach to both bioweapons and emerging infectious diseases (Fidler, 2003b). Bush administration policy on national and homeland security includes attention on, and funding for, defence against bioterrorism (White House, 2002b; Office of Homeland Security, 2002). Perhaps more surprising is the Bush administration’s neo-Westphalianism concerning emerging infectious diseases, something the previous two Republican administrations did not exhibit. The administration conceives of HIV/AIDS, for example, as a threat to U.S. national security and foreign policy objectives, including fighting global terrorism, promoting trade liberalisation, increasing stability in hard-hit regions (eg sub-Saharan Africa), working with key powers such as China, supporting economic development in poor countries, and advancing democracy globally (White House, 2002a, pp 10, 19, 22-23, 27). This neo-Westphalian approach to HIV/AIDS explains why the Bush administration’s proposed USD 15 billion, five-year Emergency Plan for AIDS Relief (Emergency Plan) represents more than humanitarianism but forms part of a strategic outlook on the exercise of US power (Bush, G, 2003a). Secretary of State Colin Powell (2003) argued that ‘[r]esponding to HIV/AIDS is not only a humanitarian and a public health issue; HIV/AIDS also carries profound implications for prosperity, democracy and security.’ President Bush (2003b) stressed the strategic nature of the Emergency Plan when he compared it to the Marshall Plan, the Berlin Airlift, and the Peace Corps.
The Bush administration’s integration of health into foreign policy does not, however, stop with its neo-Westphalianism. This administration also has a human rights perspective on global health, but one that differs from the post-Westphalianism utilised by President Carter (Fidler, D,2003b). The Bush administration sees HIV/AIDS, for example, as a threat to ‘the non-negotiable demands of human dignity’: the rule of law; limits on the absolute power of the state; free speech; freedom of worship; respect for women; religious and ethnic tolerance; and respect for private property. Health is not one of the non-negotiable demands of human dignity because the Bush administration opposes thinking about health in terms of economic, social, and cultural rights. For the Bush administration, poor health and epidemics can threaten civil and political rights rather than the right to health. Health finds human-rights meaning as an important material input into the enjoyment of individual liberty.
The Bush administration re-writes the substantive meaning of post-Westphalianism, replacing the right to health with health as a central concern for the exercise of civil and political rights. The solidarism that flows from the Bush rights position is solidarity grounded in individual liberty not health, and universal justice is not measured by redistributed wealth but by the security of the non-negotiable demands of human dignity in each nation. Wealth redistribution is required in this conception of post-Westphalianism, as illustrated by the Bush administration’s proposed Emergency Plan, the ‘largest, single up front commitment in history for an international public health initiative involving a single disease’ (Bush, G,2003b).
Global health’s political revolution finds, thus, the hegemon engaged in health as foreign policy on both neo-Westphalian and unique post-Westphalian terms. Even those not prone to praise the Bush administration acknowledge that its stance on HIV/AIDS is groundbreaking. Kristof (2003, p A31) argued, for example, that ‘Mr Bush is doing more about AIDS in Africa than President Clinton ever did.’ The hegemon’s engagement involves not only proposals for increased U.S. contributions to global health (Bush, G, 2003a) but also the integration of the HIV/AIDS threat into overall national security and foreign policy objectives (White House, 2002a).
The Bush administration has taken health as foreign policy beyond the ‘soft power leadership role’ advocated by Kickbusch (2002, p 139) because it has conceptualised health threats as directly relevant to hard and soft power interests of the United States. The unprecedented nature of the Bush administration’s incorporation of health into US foreign policy has, nevertheless, generated controversy for two basic reasons. First, many global health advocates are unhappy with the Bush administration’s health unilateralism, expressed in its emphasis on domestic bioterrorism preparedness (Vedantam, S, 2003, p A08) and the manner in which it approaches the global HIV/AIDS problem (eg distributing the vast majority of the Emergency Plan’s proposed sums bilaterally rather than through the Global Fund) (Fidler, D, 2003d, p 141). Second, critics believe more is needed from the United States, particularly financially, than the Bush administration has promised or delivered because the magnitude of global infectious disease problem is enormous (Fidler, D, 2003d, p 142-43).
In sum, global health’s political revolution involves the germ threat influencing how the world’s hegemon conceptualises national security and foreign policy and how it exercises material power. Global health concerns are not determining how the United States exercises its power; but, under Bush administration policy, the United States cannot exercise its power today without confronting the global germ threat, whether the issue is homeland security, trade liberalisation, aid to sub-Saharan Africa, or the axis of evil.
Interestingly, the Bush administration has given the germ threat, especially HIV/AIDS in developing countries, such a significant profile that it cannot, if it is sincere, afford to have its neo-conservative approach found wanting. Referring to the Emergency Plan, Kristof (2003, p A31) warned that, unless President Bush ‘delivers on his promises, then it will all look like the most cynical of gestures—using the great health tragedy of our age as a cheap photo-op to drape the White House in compassion.’ The United States itself has raised the stakes of global health’s political revolution in framing the germ threat in a manner that requires, practically and philosophically, the serious engagement of US power.
5. Dilemmas in Global Health’s Political Revolution
Analysis of the components of global health’s political revolution—germs, norms, and power—reveals the transformation of an area from obscurity to national security, neglect to neo-conservatism, and humanitarianism to hegemonic engagement. The revolution is, however, troubling because unresolved dilemmas arise with respect to each component; and these dilemmas combine to create uncertainty as to what direction ‘health as foreign policy’ will take in the 21st century.
As indicated earlier, revolutions involve crises with the status quo. For global health, the crisis has been the threat posed by pathogenic microbes. From a public health perspective, this crisis is, at best, a mixed blessing. The microbial menace contains a disturbing message: public health is now more politically important because infectious diseases are menacing. Most public health experts would trade global health’s political revolution for an environment lacking a germ threat that shows no signs of abating. The germs dilemma suggests that public health’s political importance depends on the existence of severe infectious disease problems, which are evidence of public health failures.
Neo-Westphalianism’s strength in foreign policy debates about infectious diseases underscores the germs dilemma. Neo-Westphalianism reveals concern on the part of the great powers about global health problems, but this concern only arises in connection with disease threats serious enough to threaten such powers directly and indirectly. Threats of this magnitude, such as HIV/AIDS, expose public health failures on a global basis. Further, does the attention of the great powers wane when the germ threat abates, producing another cycle of complacency and crisis? The germs dilemma raises doubts about whether global health has transformed the dynamics of foreign policy and international relations.
The ferment in normative thinking about the germ threat also contains a problem that connects to the germs dilemma. The potential for the GHG/GPGH strategy to provide concurrency between neo-Westphalianism and contemporary post-Westphalianism depends on the global infectious disease problem being serious enough to activate neo-Westphalianism. This dynamic means health as foreign policy may have limited scope, restricted to significant epidemics of direct (eg SARS) and of indirect concern (e.g., HIV/AIDS pandemic) to strong countries. Such restricted scope cuts against the rights-based universalism of post-Westphalianism, reducing this normative perspective’s potential to contribute to concurrency through GHG/GPGH strategies.
Critics have argued, for example, that GPGH represent a consequentialist strategy unsuited to fostering communitarian concern for the health of poor populations and individuals (Mooney, G and Dratzor, J, 2003, p 241). The lack of common ground between the utilitarian neo-Westphalianism and the deontological post-Westphalianism limits the concurrency GHG/GPGH strategies can achieve. This situation leaves global health’s political revolution facing normative indeterminacy and vulnerable to the normative preferences of the most powerful. The Bush administration’s embrace of neo-Westphalianism and replacement of post-Westphalianism with its neo-conservative perspective on health and human dignity illustrate this aspect of the norms dilemma. The larger implication of the norms dilemma is that power determines the norms applied to global health rather than norms controlling power exercised for global health.
Responding to the germ threat requires the application of material resources that can only realistically come from the great powers. The need for power gives those with power leverage over what germs are confronted and on what normative basis such confrontations take place. The need for power re-establishes borders in the context of an increasingly borderless problem. A world in which U.S. power is preponderant exacerbates this dilemma. Many advocates for global health are caught in the power dilemma: they must appeal for US engagement using arguments from US self-interest, but they dislike the engagement when it actually occurs.
The power dilemma today’s world also connects to the germs dilemma. For a hegemonic power to be threatened by germs, the germ threat has to be significant. The Clinton administration did not conceptualise HIV/AIDS as a national security threat until after the extent of the HIV/AIDS pandemic had become nearly catastrophic in sub-Saharan Africa. Likening the Emergency Plan to the Marshall Plan reveals the presence of societal devastation of historic proportions.
Combined, the germs, norms, and power dilemmas raise questions concerning the meaning and sustainability of global health’s political revolution. This revolution has elevated the foreign policy importance of global health, but what is less clear is whether this importance means health has transformed foreign policy or whether foreign policy has co-opted health. Post-Westphalianism contains a vision of health transforming foreign policy in placing the individual at the centre of attention, stressing health solidarism among nations, and effecting redistributive justice. By contrast, neo-Westphalianism embeds health into traditional foreign policy conceptions and transforms health into materiél for the machinations of states. GHG/GPGH concepts create a hybrid strategy that can appeal to post-Westphalian and neo-Westphalian approaches but overcome neither.
Although the germs, norms, and power dilemmas indicate that neo-Westphalianism is prominent, two developments suggest that ‘health as foreign policy’ in the future may not be entirely neo-Westphalian. First, the demonstration of the power of GHG/GPGH strategies during the SARS outbreak indicates that these strategies have potential sustainability in global health’s political revolution. Second, the Bush administration’s neo-conservative approach gives health a strategic and philosophical importance that may keep global health higher on the agenda of the hegemon and world politics than would be expected from strict neo-Westphalianism.
When asked about the French Revolution’s impact, 20th century Chinese statesman Chou En-Lai responded that it was too early to tell. It is also too early to tell the ultimate direction and meaning of global health’s enigmatic political revolution. The interdependency among germs, norms, and power is still sufficiently volatile to prevent confident predictions about the future.
Mapping global health’s political revolution against leading theories of international relations provides a sense of this volatility. Although Westphalianism’s prominence in the revolution echoes Realpolitik teachings about international politics, the germ threat from emerging infectious diseases and bioterrorism falls outside the Realpolitik framework because it is not, strictly speaking, a material threat posed by states. Contemporary post-Westphalianism resonates with constructivism’s assertions that ideas, not just power, influence international relations. The Bush administration’s linkage of the HIV/AIDS pandemic to the protection and promotion of individual rights, democracy, and economic interdependence recalls liberal theory on international relations. The GHG/GPGH concepts touch on themes found in institutionalism, with its emphasis on the importance of international institutions and regimes, and liberalism, with its embrace of non-state actors as legitimate governance participants.
The difficulty confronted in slotting global health’s political revolution into existing theories of world politics suggests that this revolution has more theoretical and practical importance for foreign policy and world politics than has been appreciated to date. The enigma of global health’s political revolution provides a microcosm of the enigma of managing globalized anarchy in the 21st century.
At present, one thing is clear: the germs will keep coming. The continuation of the germ threat will keep norms in ferment and power engaged. Although well underway, global health’s political revolution may have only just begun. Danger and opportunity await.
Endnotes
1The term ‘Westphalian’ derives from the Peace of Westphalia of 1648, which scholars consider a landmark moment in the history of international relations because the Peace of Westphalia, in ending the Thirty Years’ War, established principles that dominated the structure and dynamics of international relations for the next three centuries. Three core principles of the Westphalian international system are state sovereignty, non-intervention in the domestic affairs of other states, and regulation of state interaction through consent-based rules of international law.
References
Arhin-Tenkorang, D and Conceição, P (2003) ‘Beyond Communicable Disease Control: Health in the Age of Globalization,’ in Kaul I, Conceição P, Le Goulven K, and Mendoza RU (eds), Providing Global Public Goods: Managing Globalization (Oxford: Oxford University Press).
Ban, J (2001) Health, Security, and US Global Leadership (Washington, DC: Chemical and Biological Arms Control Institute).
Beaglehole, R and Yach, D (2003) ‘Globalisation and the Prevention and Control of Non-Communicable Disease: The Neglected Chronic Diseases of Adults’, The Lancet 362, pp 903-08.
Brower, J and Chalk, P (2003) The Global Threat of New and Reemerging Infectious Diseases: Reconciling U.S. National Security and Public Health (Santa Monica: RAND).
Bush, G (2002) ‘State of the Union Address’ < http://www.whitehouse.gov/news/releases/2002/01/20020129-11.html>.
Bush, G (2003a) ‘State of the Union Address’ < http://www.whitehouse.gov/news/releases/2003/01/20030128-19.html>.
Bush, G (2003b) ‘Remarks by the President on Signing H.R. 1298, the U.S. Leadership Against HIV/AIDS, Tuberculosis, and Malaria Act of 2003’ <http://www.state.gov/oes/rls/rm/2003/20986.htm>.
Campbell, K M and Zelikow, P (eds) (2003) Biological Security & Public Health: In Search of a Global Treatment (Washington, DC: Aspen Institute).
Committee on Economic, Social, and Cultural Rights (2000) General Comment 14 on the Right to the Highest Attainable Standard of Health, U.N. Doc. E/C.12/2000/4.
Center for Strategic and International Studies (2002) Contagion and Conflict: Health as a Global Security Challenge: A Report of the Chemical and Biological Arms Control Institute and the CSIS International Security Program (Washington, DC: Center for Strategic and International Studies).
Dodgson, R, Lee, K and Drager, N (2002) Global Health Governance: A Conceptual Review (London: Centre on Global Change and Health and WHO).
Farmer P (1999) Infections and Inequalities: The Modern Plagues (Berkeley: University of California Press).
Fidler, D (2003a) ‘International Law and Weapons of Mass Destruction: The End of the Arms Control Approach?’ Duke International and Comparative Law Journal (in press).
Fidler, D (2003b) ‘Caught Between Paradise and Power: Public Health, Pathogenic Threats, and the Axis of Illness’, McGeorge Law Review (in press).
Fidler, D (2003c) ‘Fighting the Axis of Illness: HIV/AIDS, Human Rights, and U.S. Foreign Policy’, Harvard Human Rights Journal (in press).
Fidler, D (2003d) ‘Racism or Realpolitik? U.S. Foreign Policy and the HIV/AIDS Catastrophe in Sub-Saharan Africa’, Journal of Gender, Race & Justice 7, pp 97-146.
Fidler, D (2004) SARS, Governance and the Globalization of Disease (London: Palgrave Macmillan).
Foege, W (2003) ‘Memorandum to the President: Global Health and U.S. National Interests,’ in Campbell K and Zelikow P (eds) Biological Security & Public Health: In Search of a Global Treatment (Washington, DC: Aspen Institute).
Garrett, L (1995) The Coming Plague: Newly Emerging Diseases in a World Out of Balance (New York: Penguin Books).
Goodman, N (1971) International Health Organizations and Their Work, 2nd ed, (London: Churchill Livingstone).
Gruskin, S and Tarantola, D (2003) ‘Health and Human Rights,’ in Detels R et al (eds) The Oxford Textbook of Public Health, 4th ed. (Oxford: Oxford University Press).
Howard-Jones, N (1975) The Scientific Background of the International Sanitary Conferences 1851-1938 (Geneva: WHO).
Hunt, P (2003) The Right of Everyone to the Enjoyment of the Highest Attainable Standard of Physical and Mental Health: Report of the Special Rapporteur, U.N. Doc. E/CN.4/2003/58.
Lee, K and Zwi, A (2003) ‘A Global Political Economy Approach to AIDS: Ideology, Interests and Implications’ in Lee, K (ed) Health Impacts of Globalization: Towards Global Governance (London: Palgrave Macmillan).
Institute of Medicine (1992) Emerging Infections: Microbial Threats to Health in the United States (Washington, DC: National Academy Press).
Institute of Medicine (1997) America’s Vital Interest in Global Health: Protecting Our People, Enhancing Our Economy, and Advancing Our International Interests (Washington, DC: National Academy Press).
Institute of Medicine (2003) Microbial Threats to Health: Emergence, Detection, and Response, ed. Smolinski, M, Hamburg, M and Lederberg, J (Washington, DC: National Academy Press).
Kassalow J (2001) ‘Why Health is Important to U.S. Foreign Policy’ <http://www.milbank.org/Foreignpolicy.html>.
Kaul, I, Grunberg, I and Stern, M (eds) (1999) Global Public Goods: International Cooperation in the 21st Century (Oxford: Oxford University Press).
Kessler, G and Stein, R (2003) ‘Powell Says U.S. Leading Effort on AIDS,’ Washington Post, 23 September 2003, p A24.
Kickbusch, I (2002) ‘Influence and Opportunity: Reflections on the U.S. Role in Global Public Health,’ Health Affairs, 21, pp 131-41.
Kickbusch, I (2003) ‘Global Health Governance: Some Theoretical Considerations on the New Political Space’ in Lee, K (ed) Health Impacts of Globalization: Towards Global Governance (London: Palgrave Macmillan).
Kristof, N (2003) ’When Prudery Kills’ New York Times, 8 October 2003, p A31.
Koplow, D (2003) Smallpox: The Fight to Eradicate a Global Scourge (Berkeley: University of California Press).
Mooney G, Dratzor J (2003) ‘Global Public Goods for Health: A Flawed Paradigm?’, in Smith, R, et al (eds) Global Public Goods for Health: Health Economic and Public Health Perspectives (Oxford: Oxford University Press).
National Intelligence Council (2000) The Global Infectious Disease Threat and Its Implications for the United States. National Intelligence Estimate 99-17D, <http://www.cia.gov/cia/publications/nic/report/nie99-17d.html>.
National Science and Technology Council Committee on International Science, Engineering, and Technology (CISET) Working Group on Emerging and Re-Emerging Infectious Diseases (1995) Infectious Diseases—A Global Health Threat (Washington, DC: CISET).
Powell, C (2003) Remarks at Bill Signing Ceremony for the US Leadership Against HIV/AIDS, Tuberculosis, and Malaria Act of 2003, 27 May 2003, <http://www.state.gov/secretary/rm/2003/20969.htm>.
Smith, R, et al (eds) (2003) Global Public Goods for Health: Health Economic and Public Health Perspectives (Oxford: Oxford University Press).
Thomas, C (2003) ‘Trade Policy, the Politics of Access to Drugs and Global Governance for Health,’ in Lee, K (ed) Health Impacts of Globalization: Towards Global Governance (London: Palgrave Macmillan).
UNAIDS (2001) 20 Years of AIDS (on file with author).
US Centers for Disease Control and Prevention (CDC) (1994) Addressing Emerging Infectious Disease Threats: A Prevention Strategy for the United States (Washington, DC: Department of Health and Human Services).
US Centers for Disease Control and Prevention (CDC) (1998) Preventing Emerging Infectious Diseases: A Strategy for the 21st Century (Washington, DC: Department of Health and Human Services).
Vedantam, S (2003) ‘WHO Assails Wealthy Nations on Bioterror: Coordination of Defenses Poor in Simulation; U.S. Support for Agency Questioned,’ New York Times, 5 November 2003, p A08.
White House (1978) New Directions in International Health Cooperation (Washington, DC: The White House).
White House (2002a) The National Security Strategy of the United States of America (Washington, DC: The White House).
White House (2002b) National Strategy to Combat Weapons of Mass Destruction (Washington, DC: The White House).
World Health Organisation (1948) ‘Constitution of the World Health Organization,’ in WHO, Basic Documents, 40th ed. (Geneva: WHO, 1994).
World Health Organisation (1978) Primary Health Care: Report of the International Conference on Primary Health Care, Alma-Ata, USSR, 6-12 September 1978 (Geneva: WHO).
World Health Organisation (1999) Removing Obstacles to Healthy Development (Geneva: WHO).
World Health Organisation (2002a) Global Defense Against the Infectious Disease Threat, Kindhauser, M (ed) (Geneva: WHO).
World Health Organization (2002b) Global Crises—Global Solutions: Managing Public Health Emergencies of International Concern Through the Revised International Health Regulations (Geneva: WHO).
World Health Organization (2003) Revision of the International Health Regulations, WHO Doc. WHA56.29, 28 May 2003.
Zelikow (2000) ‘Book Review,’ Foreign Affairs 79(4), p 154.
